What is Parksinson’s Disease? How can Physical, Occupational, and Speech Therapy help?
- F.I.T. PT

- Dec 1, 2021
- 3 min read
Updated: Jan 30, 2023
Background of Parkinson’s Disease

Parkinson’s disease is a neurodegenerative disorder that affects the neurons of the substantia nigra, a basal ganglia (a cluster of subcortical nuclei) structure located in the midbrain. The substantia nigra regulates voluntary motor movements and muscle control. The nerve cells of the basal ganglia and substantia nigra produce dopamine, a neurotransmitter, that controls voluntary movement, emotions, cognitive planning, and cognition and learning. When the subcortical nuclei are damaged it can result in neurological conditions, such as Parkinson’s disease, Huntington's disease, Obsessive-Compulsive Disorder, Attention Deficit Hyperactivity, Schizophrenia, and Tourette syndrome. Neurons in the brain begin to break down or die, causing levels of dopamine to decrease, leading to loss of motor movements due to abnormal brain activity.
Symptoms
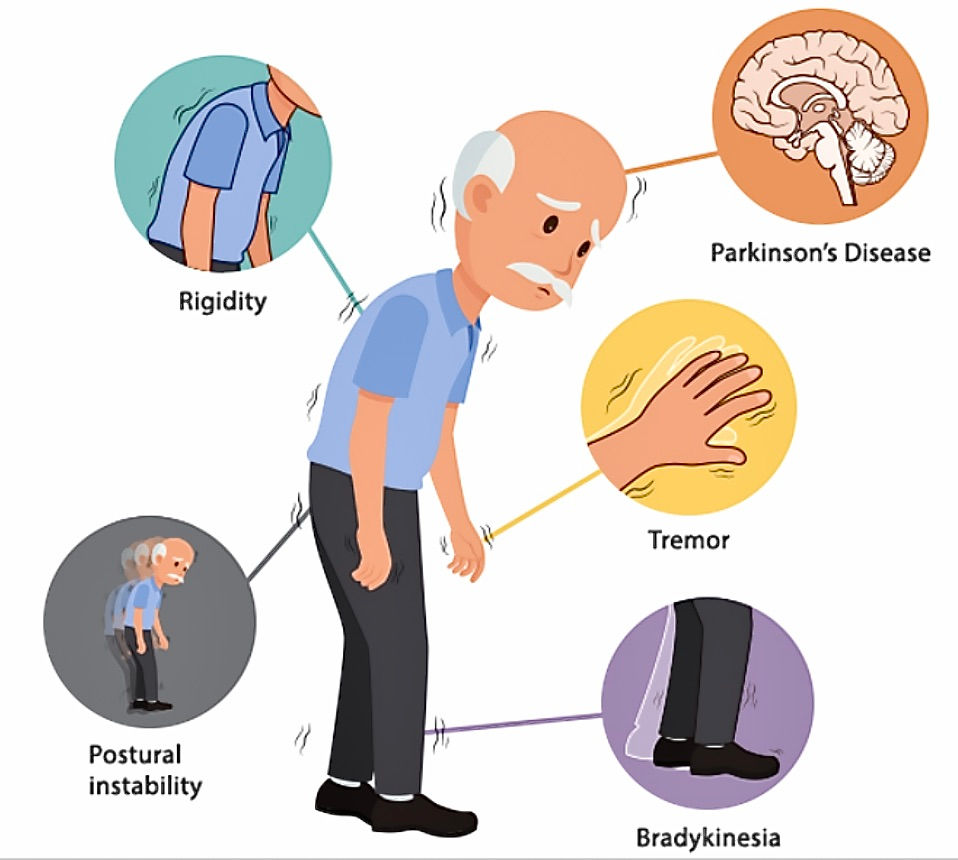
The symptoms of Parkinson’s disease vary in intensity per person. In the beginning, the symptoms can go unnoticed or be mild, for instance, one may experience tremors in one of their hands or fingers. As time progresses, one’s symptoms begin to worsen and affect both sides of the body. The signs and symptoms of Parkinson’s disease include:
Tremors
Bradykinesia
Rigid muscles
Impaired posture (gait) and balance
Loss of involuntary movements
Speech changes
Handwriting changes

The disease can progress over time and symptoms can worsen without proper management.
Gait, Motor Function, and Balance
Loss of dopaminergic innervation of the basal ganglia in Parkinson’s disease leads to changes in gait and balance. The changes in voluntary motor movements restrict functional independence. There are two classifications of gait disturbances: continuous and episodic. Episodic gait disturbances occur intermittently and in a random, inexplicable manner. Continuous gait disturbances are seen in patients with advanced Parkinson’s disease. It is described as alterations in a walking pattern similar to small shuffling steps accompanied by slow movement, called hypokinesia, in extreme cases, one may experience a complete loss of movement (akinesia).
The loss of control of the body’s center of mass is the definition of balance. The nervous and musculoskeletal system sends the brain information to carry out balance control- moving and standing still. Postural instability (balance issues) is one of the main motor symptoms identified in patients with Parkinson’s disease. There are various degrees in severity accompanied by progression of the disease. Postural instability can be witnessed and experienced when rising from a chair, rising from a bed, standing upright, and turning (especially with quick movements). A decrease in the ability to balance causes an increase in falls which can lead to an increase in hospitalizations. Tremors, rigidity (stiffness of a limb(s) or body), and bradykinesia (loss of spontaneous movement) are the other three primary motor symptoms experienced by patients with balance issues.
How Can Physical, Occupational, and Speech Therapy help if you or a family member is living with Parkinson’s Disease?
Occupational Therapy:
Occupational therapists will assist you in performing everyday activities with ease and the intent to help you maintain your independence. Your occupational therapists will introduce you to different ways to complete tasks and introduce new equipment that you can use. During your initial consultation, your Occupational Therapist will perform an assessment, establish an individualized treatment plan, and recommend suggestions in the following areas:
Upper extremity strength and mobility
Handwriting aids
Home modification
Vehicle modification information
Feeding and utensil adaptations
Maximize energy consumption
Computer and workplace modifications
Leisure activity skill development
Bathroom equipment installation/use
Grooming and dressing aids
Physical Therapy:
If you have Parkinson’s Disease, with Physical Therapy, you can learn how to better participate in your daily tasks and have a better quality of life. Your physical therapist at F.I.T. PT will teach you new movement techniques and strategies as well as how to use equipment recommended for your home, workspace, and vehicle. Your therapist will teach you exercises to help strengthen your muscles, improve balance and coordination, relieve pain, increase mobility, and preserve energy. The goal is to maintain your independence and improve your quality of life.
Speech Therapy:
One of the many symptoms of Parkinson’s Disease is difficulty speaking and swallowing (dysarthria and dysphagia). Seeking services from our Speech Therapist at F.I.T. PT will help you learn ways to conserve energy and maintain communication skills, both verbal and non-verbal. During the consultation and therapy sessions, your Speech Therapist will help you with swallowing difficulties, speech and language deficits, and communication issues.
References
Beato, M.R., Reddy, V., & Sonne, J., (2020). Neuroanatomy, substantia nigra. StatPearls
Publishing. Retrieved November 20, 2021, from
Downward, E. (2017, February 28). Motor symptoms of parkinson’s. Parkinson’sDisease.net.
Downward, E. (2017, February 28). Symptoms- postural instability and balancing issuees.
ParkinonsDiease.net. https://parkinsonsdisease.net/symptoms/balancing-issues-postural-
Instability
Elkouzi, A. (2021). What is parkinson’s?. Parkinson’s Foundation.
Hausdorf, J.M. (2009). Gait dynamics in parkinson’s disease: common and distinct behavior
among stride length, gait variability, and fractal-like scaling. CHAOS: An Interdisciplinary
Journal of Nonlinear Science, 19(2), 026113-1-026113-14. https://doi.org/10.1063/1.3147408
Melinosky, C. (2020, October 29). Parkinson’s disease and speech therapy. WebMD.
Melinosky, C. (2020, October 29). Physical and occupational therapy for parkinson’s disease.
Midbrain. (2019, November 13). Brain Made Simple. https://brainmadesimple.com/midbrain/




My husband was diagnosed of Parkinsons disease 2 years ago, when he was 49. He had a stooped posture, tremors, right arm does not move and also a pulsating feeling in his body. He was placed on Senemet for 8 months and then Sifrol was introduced and replaced the Senemet, during this time span he was also diagnosed with dementia. He started having hallucinations, lost touch with reality. Suspecting it was the medication I took him off the Siferol (with the doctor’s knowledge) and started him on PD-5 natural herbal formula we ordered from AKNNI HERBAL CENTRE, his symptoms totally declined over a 3 weeks use of the AKANNI HERBAL Parkinsons disease natural herbal formula. He is now almost 51…
At the age of 66, my spouse was diagnosed with Parkinson's disease. His symptoms included excruciating calf pain, muscular aches, tremors, slurred speech, frequent falls, loss of balance, and trouble standing up from a seated posture. After six months on Senemet, Siferol was given to him in place of the Senemet. It was also at this period that he was diagnosed with dementia. He began seeing hallucinations and became detached from reality. With the doctor's approval, we stopped giving him Siferol and chose to try the Natural Herbs Center PD-5 program, which we had previously investigated. After three months of therapy, he has made significant progress. The illness has been completely contained. There are no symptoms of persistent twitching, weakness,…